|
--- By Erica Sastre, LMT  Yes! Chiropractic has been proven to help manage both acute and chronic pain. Pain management, in general, is a big issue in healthcare. Let’s look at some facts: Low back pain is the single leading cause of disability. According to the US bone and Joint initiative study, back pain was cause for over 264 million days off of work. That is all without considering any other type of chronic pain condition. Pain affects more Americans than diabetes, heart disease and cancer combined. When looking for solutions to chronic pain, the first thing we tend to reach for is over-the-counter aids such as Aspirin, Advil, or Ibuprofen. Then if these conditions worsen and we go to the doctor we are typically directed to stronger prescription medications, which, can be concerning to many patient situations. Many people are looking for ways to treat their chronic pain without resorting to drugs of the traditional medication protocol. With alternative care we can lessen our dependency on over the counter drugs and even opioids.  Back pain is also one of the most common conditions that opioids are prescribed for with over half of opioid users reporting back pain among their symptoms. Why is this connection between back pain and opioids so concerning? While prescription opioids are certainly helpful to many patients in complex severe conditions, however, we need to also be looking at the big picture of the opioid crisis: In 2016, illicit and prescription opioids were responsible for more than 42,000 fatal overdoses across the country. According to the Centers of Disease Control and Prevention, those numbers have quintupled since 1999, which means the problem is just getting worse. The good news is that, alternative medicines are already making great improvements to these dire statistics.  Let's take a look at some strategies the VA has been using in order reduce opioid addiction among veterans. After launching one initiative, they were able to reduce overall opioid prescriptions by 41% over the past five years. The project was focused on non-drug treatment for chronic pain, such as acupuncture, spinal manipulation therapy, chiropractic care, and yoga. It is also good news to know that patients who received services from a chiropractor were less likely to fill a prescription for opioid medication, and, there was a 51 percent lower likelihood of an adverse drug incident compared to non recipients of chiropractic care. 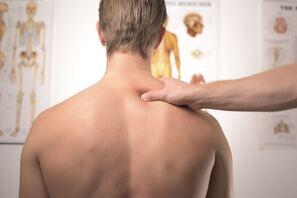 A visit to the chiropractor may also be more cost effective for sufferers of chronic pain. In one study, "those who initiated treatment for low back pain with chiropractic rather than a regular MD had 40% in reduced healthcare cost!" In general “Healthcare plans that incorporate chiropractic typically realize a 2:1 return for every dollar spent.” There are numerous research studies, reports, and surveys proving how effective chiropractic can be for pain: "In a Randomized controlled trial, 183 patients with neck pain were randomly allocated to manual therapy (spinal mobilization), physiotherapy (mainly exercise) or general practitioner care (counseling, education and drugs) in a 52-week study. The clinical outcomes measures showed that manual therapy resulted in faster recovery than physiotherapy and general practitioner care. Moreover, total costs of the manual therapy-treated patients were about one-third of the costs of physiotherapy or general practitioner care." Korthals-de Bos et al (2003), British Medical Journal “Patients with chronic low-back pain treated by chiropractors showed greater improvement and satisfaction at one month than patients treated by family physicians. Satisfaction scores were higher for chiropractic patients. A higher proportion of chiropractic patients (56 percent vs. 13 percent) reported that their low-back pain was better or much better, whereas nearly one-third of medical patients reported their low-back pain was worse or much worse.” Nyiendo et al (2000), Journal of Manipulative and Physiological Therapeutic The evidence and anecdotes are solid. If you are suffering form chronic or acute pain, chiropractic care may well worth a try! Send us your questions! Yours might be answered next week. [email protected] Sources and Further Reading:
NIH Fact Sheet -- Pain Management The Center for Disease Control and Prevention -- Drug Overdose Deaths VHA Pain Management -- Opioid Saftey Initiative Boss Magazine -- Corrective Care for the Opioid Epidemic American Chiropractic Association -- What Research Shows About Chiropractic
2 Comments
-- By Erica Sastre, LMT 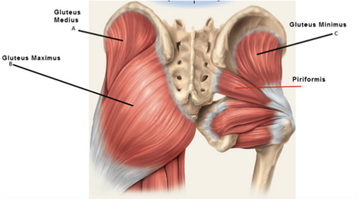 Did your massage therapist hit a particularly tender spot in your glutes? Did you have pain or tingling running down your leg? Why is your chiropractor trying to make you do so many squats? This week we are putting the spotlight on the piriformis muscle! The piriformis muscle is a muscle under the gluteus maximus, it attaches at the anterior surface of the sacrum, and the superior aspect of the greater trochanter (SI joint to the top of the femur). It Latterally rotates the hip (twists your thigh outward) , and abducts the hip when the hip his flexed (pulls your thigh away from the body center-line). 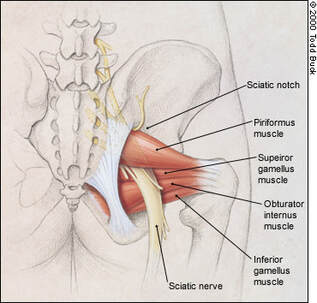 What could possibly go wrong? Piriformis can be a literal pain-in-the-butt! A tight or knotted up piriformis muscle can cause pain on its own, or limit strength and flexibility. However, this small muscle can cause much bigger problems. The Piriformis is often to blame for sciatic pain symptoms. The sciatic nerve runs right past the piriformis muscle, and sometimes even through the piriformis muscle. Due to its placement in the body, tightness in the piriformis and adjacent muscles can pinch the sciatic nerve. This can send pain, numbness, or tingling down all or parts of the leg! If you have ruled out a spinal issues as your source of sciatic, it's time to address the piriformis muscle. How does the piriformis affect my posture? Check out your toes! If your feet tend to turn in when you are standing, walking, running, or squatting you may have a weak piriformis muscle. Likewise, if you see that your feet tend to turn outward when standing, walking, running, or squatting, it may be a sign that your piriformis is overdoing it. Either one of these postures can cause problems in the legs, hips and knees, especially with load-bearing exercise. Squatting and lifting weights with misalignment can spell disaster for the knees! Keep in mind that if it is a hip/piriformis weakness, the positional problem will originate from where the hip and thigh meet. If the positional problem originates in the knee or ankle, we will have other muscles to look at! That's why it's a good idea to see a professional, like your chiropractor, to help evaluate postural problems. How do I stretch it? Pigeon pose is everyone’s favorite piriformis stretch! There are a number of modified pigeon poses you can try if you are less flexible. If floor stretches are uncomfortable, try doing a pigeon pose on a chair, couch, or low table. The 'figure 4' can be done sitting or supine (on your back), or even standing if you have good balance! How do I strengthen it? Piriformis is a lateral rotator. Meaning, it twists the thigh 'outward' from your hip. Working the gluteal region will generally build the piriformis, as well as create support for the piriformis with the other gluteal muscles. Squats are an easy way to develop the glutes. Add a band for extra resistance! Try a one-legged dead lift and keep in mind that the grounded leg is the piriformis that you are strengthening. Work one leg at a time, grab on to the back of a chair, bar, or ledge. Lift the other leg out to the side, you can do this exercise with your feet paralell (both toes facing forward) or 'turned out' (feet make a V shape with your toes pointing outward, like in ballet). Try this one with a band as well! 'Fire Hydrant' starts on all fours. Keep your knee at 90 degrees then swing your leg out to the side, keeping your frame strong to isolate and work the glutes. Fun facts about the piriformis
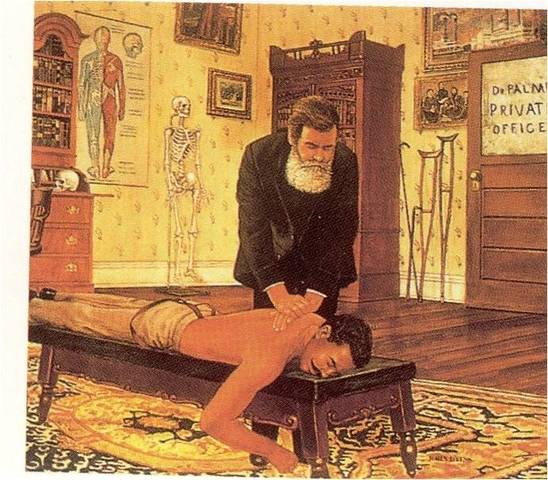
The piriformis is only one of six muscles in the lateral rotator group. The others are; gemellus superior, obturator internus, gemellus inferior, quadratus femoris and the obturator externus. In 17% of the population the piriformis muscle is pierced by all or part of the sciatic nerve. The word piriformis comes from latin, meaning ‘pear shaped’. Hopefully you learned something fun about the piriformis today! Stay tuned for our next Q&A, and send your questions to [email protected]! What muscle should we feature next? -- by Erica Sastre, LMT A: The answer is… Probably! Let’s be honest, most of the time the answer is yes. Even if it is not the root cause of your back pain, wearing a backpack incorrectly can seriously worsen other conditions such as disc herniation, scoliosis, hip and shoulder disorders. Most people wear backpacks improperly, or are overloading their backs. How heavy are our backpacks? School books are just the beginning of spinal stress for students, most of whom are doing extracurricular activities. Imagine a 30 pound backpack, a tuba, a poster board presentation, and a soccer bag that all need to be transported to and from school! How heavy is ‘too’ heavy? “The American Academy of Pediatrics recommends that a child’s backpack weigh no more than 10 to 20 percent of a child’s weight.” Yikes, textbooks add up fast! Most parents are not checking to see if their kids backpacks are weighing too much, and few students are self monitoring their posture or the weight they are carrying. They merely accept whatever the coarse-load demands of them. In addition these same students spend a lot of time studying at a desk or computer, most of their day encourages a slouched, leaning forward posture. Schools are slowly changing with the times, some students have options to have electronic books, or share books at school so they don’t need to carry so much. Each situation is different, but most still need to carry all their books, and do their best. The WRONG way to wear Backpacks The Correct Way to Wear a Backpack  Photo by Mar Bocatcat on Unsplash Photo by Mar Bocatcat on Unsplash Notice how the spine is straight, shoulders are even, hips are even. The straps are used so that weight is evenly distributed between the hips and torso! This is the part that most kids want to skip, but if you look at climbers, hikers, military, they all use straps with their packs to distribute the load properly, this helps them move more freely and prevent injury! 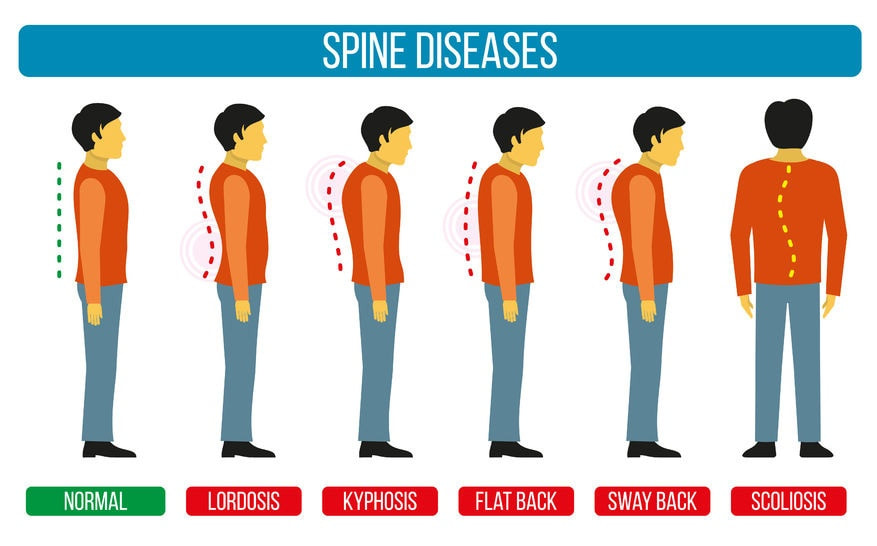 Why is this so important? Most students spine are in the process of growing! Teens are experiencing their growth spurt, some don’t finish growing until their 20’s so this concern even applies to college students. The spine is supposed to be extending upwards as it grows There is a normal amount of curvature within the spine, but not too much (which is called Kyphosis in the thoracic spine and Lordosis in the lumbar spine). Nor is it supposed to grow into a twist, or a side-to side bend (Scoliosis). If we load up the back, and twist the spine because of weight, every single day, over time we are encouraging the spine to grow in a curve or twist. It much more difficult to correct posture later in life. What can we do if our children seem to be suffering from posture problems related to their backpack? 1) Lighten the load. Two sets of textbooks, electronic textbooks, sharing books with friends. Talk to teachers and administrators to work out viable solution for your child and the other students! 2) Corrective stretches and exercises, as well as regular participation in activities that encourage correct posture and body mechanics such as yoga, dance, martial arts & climbing are all great examples. Stay tuned for next weeks Q&A! If you have any questions yourself, please feel free to send in your questions to [email protected] -- By Erica Sastre, LMT  Hey everybody, Erica here with this week's Q&A. February is Black History Month, I thought I would endeavor to learn a little about more about African American History in the Chiropractic profession. I’m kind of a history nerd, and I thought this project would be a lot of fun. Well, I learned a lot! So for this week’s Q & A I’d like to share the story of Harvey J. Lillard, the man at the heart of the chiropractic story. Harvey J. Lillard was the first chiropractic patient. The very first adjustment was performed on him, and restored his hearing. This is the miracle that blew up chiropractic interest, and established a lasting profession. The founder of Chiropractic medicine was a man named Daniel David Palmer. Dr. Palmer was not yet famous when he met Lillard. At that time he was a small-time entrepreneur in Davenport, Iowa who was trying to make a living with magnetic healing and other popular modalities of that time. Lillard owned the custodial company that took care of the building where Palmer was renting his office. Palmer heard Lillard’s story of how he lost most of his hearing. An incident that apparently was accompanied by a strange ‘popping’ noise in his spine. His daughter, relates the legend... “Chiropractic came into being because of my father. " "Evidently my father was a tale-teller. He and a man that worked for him stepped in front of D.D. Palmer’s office while my father was finishing the story. Well, Dr Palmer was reading a book. The Doctor stuck his fingers between the pages and walked out to listen to the end of the tale. The Doctor was so tickled that he hit my father in the back with a book.” -Valdenia Simons Based on the story, Palmer came up with a theorized that the deafness was related to Lillard’s spinal alignment, and offered to work with him to invent a treatment. The first adjustment was in 1895, and it cured Lillard's hearing!  “I was deaf 17 years and I expected to always remain so, for I had doctored a great deal without any benefit. I had long ago made up my mind to not take any more ear treatments, for it did me no good. Last January Dr. Palmer told me that my deafness came from an injury in my spine. This was new to me; but it is a fact that my back was injured at the time I went deaf. Dr. Palmer treated me on the spine; in two treatments I could hear quite well. That was eight months ago. My hearing remains good." - Harvey Lillard  This miracle story is the foundation of chiropractic medicine, it was used to market and legitimize the technique, which rapidly grew across the country and into an established medical profession. Little is know about the other details of Harvey Lillard's life. He had a wife and daughter, Lillard and his family left Davenport Iowa in 1907 and moved to Seattle. He was a deputy sheriff there until his death in 1925. Fun fact: He is buried in the same graveyard as Bruce Lee! His grave is much smaller than Lee's, but, if you enjoy chiropractic treatments and want to say thank you next time you are in Seattle, stop by the Lake View Cemetery and see Harvey. Sadly, despite working with Lillard on creating chiropractic, Dr. Palmer did not teach African Americans. The Palmer School of Chiropractic blatantly stated, `Negros not accepted'. All major chiropractic schools until the 1950's did not accept blacks or minorities.
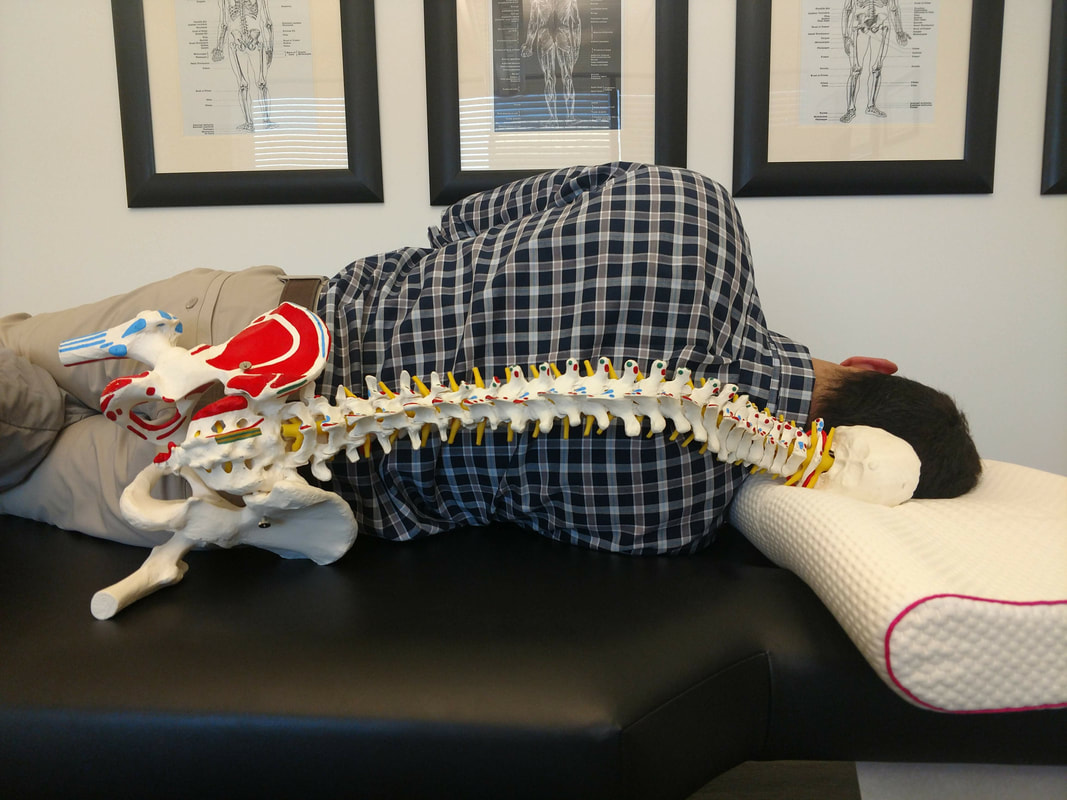
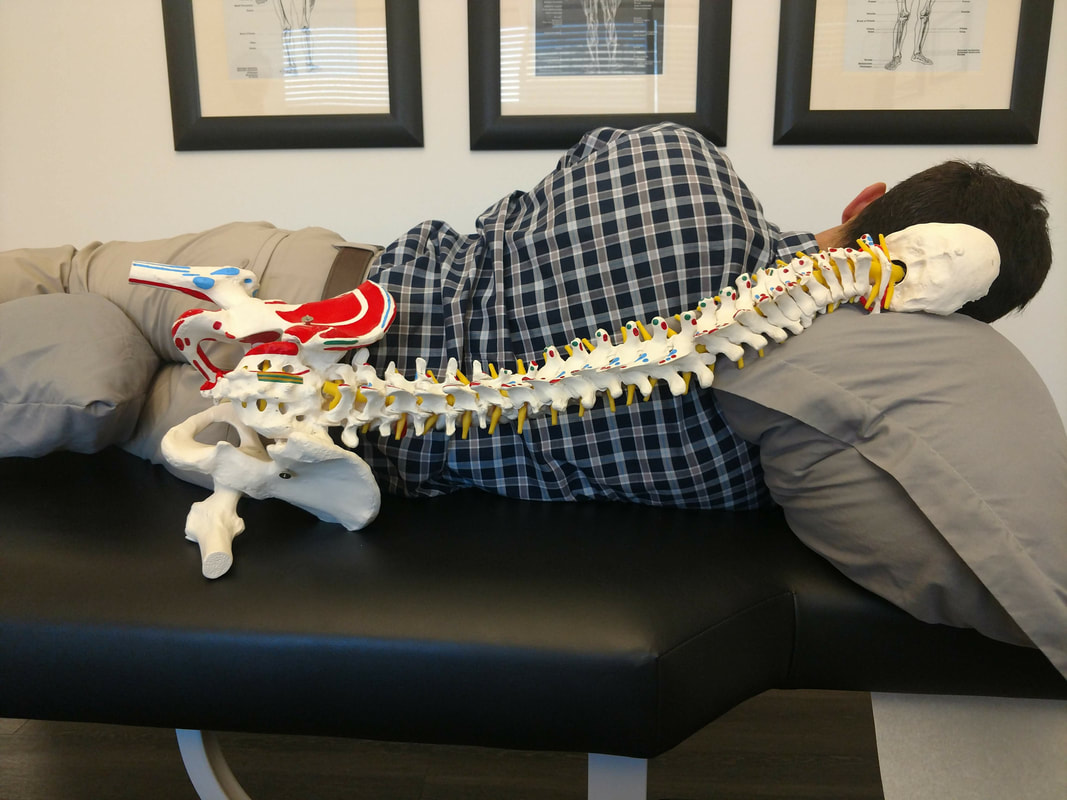
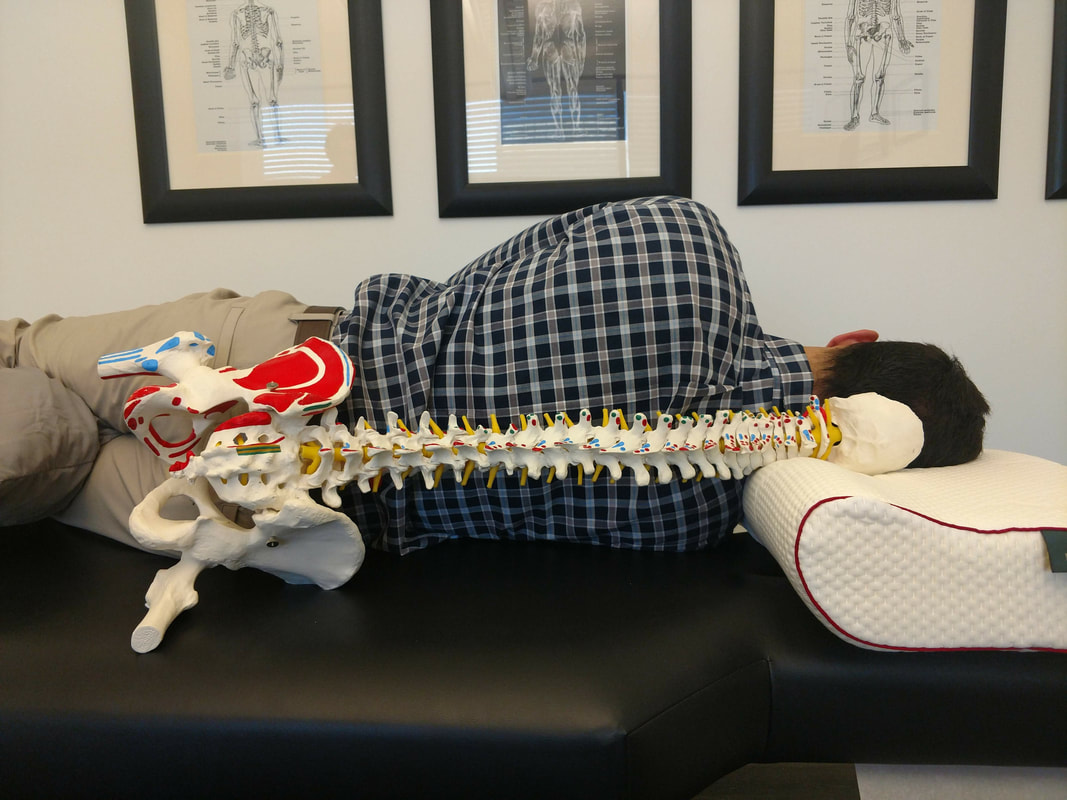
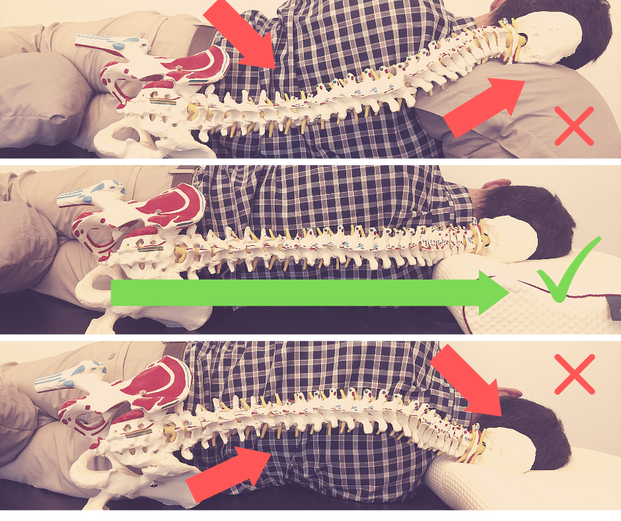
Yet, African Americans continued to participate in and contribute to the chiropractic profession. For example, Fred H. L. Rubel, established The Rubel College of Chiropractic in 1914 “to open the field of instruction to all races, no matter what the color of their skin may be, so as particularly to give members of the colored race an opportunity to learn one of the greatest modern professions—Chiropractic...” As you can see, Harvey Lillard's story was just the beginning of a rich, complex, and diverse chiropractic history. Check out this timeline to see a more complete list of events, notable figures, and facts about African American chiropractic history, check out the links below for further reading on this topic. Now we know who to thank for the chiropractic treatments we enjoy today. Don't forget to submit your own questions for us to answer! Send them [email protected], your question could be answered in next week's Q&A! --Erica Satstre, LMT -- By Jason Quieros, DC A: This answer isn’t the same for everyone. No two people should use the same pillow. The point of a pillow is to support the natural curvatures of the spine and keep it aligned throughout the night when your body is in recovery and repair mode. Sleep position plays a significant role in the type of pillow you should use. As a general rule of thumb, back sleepers should use a thinner pillow to support the head and neck, while side sleepers need a slightly larger pillow to fill in the space between the mattress and head/neck due to the width of the shoulders. It is not advised to sleep on your stomach, as it is very detrimental to both your neck and lower back resulting in pain, headaches and numbness or tingling in the arms/legs. The best way to sleep is on your back on a firm mattress which allows the spine and surrounding muscles to decompresses overnight. This also supports the natural curves of the spine and doesn’t compress any of your joints. A close alternative to sleeping on your back would be your side with the use of the proper pillows to support not only your head and neck but also your hips and shoulders. Sleeping while holding a pillow in front of you and another between your knees will allow your shoulders and hips to stay aligned, along with the spine. If you are a side-sleeper, and your pillow is too small… Neck: Your neck is forced to scrunch up and tilt downward on one side. Compressing the spinal facets and impinging nerves, blood, and muscles on this side. The other side is over stretched, and can weaken the muscles there. Over time this can create limited range of motion, neck pain, headaches, numbness and tingling in the arms, weakness, and other complications. Shoulder: Your lower shoulder is taking all the weight of your upper body. Compression of the glenohumeral joint can cause problems in the labrum, bursa, tendons and muscles of the arm and scapula, not to mention strain on the very delicate AC joint and clavicle. Spine: Your spine is is forced into an awkward ‘S’ shape. It is forced to dip down from your hips in the lumbar spine, then up over your shoulder (which remember, is bearing all this weight), then curve down again as your head weighs it down the other way. This can cause pain all on its own, and if you have any disc issues such as herniations, degeneration, or spinal impingement this sleeping position can make these more painful. Hips: Because your lumbar spine is forced up by gravity, so are your hips pulled out of alignment. This effect is worse if you don’t have a pillow between your legs. If you have sciatic pain symptoms, achy hip or knee joints, arthritis in any of these joints, take a good look at your sleep position! If your Pillow is too High… Neck: Your neck is forced up into the other direction, scrunching one side and stretching out the other. We see similar problems as with a too-small pillow. Over time you might develop thoracic outlet syndrome, neck pain, headaches, numbness/tingling in the arms, weak and or tight muscles, and limited range of motion. Shoulder: This one is a bit easier on your lower shoulder, but, it still isn’t ideal for the good ol' glenohumeral joint. Instead of your shoulders being straight across like a T, you are forcing them into a tilted angle. The upper shoulder will be dragging down on the torso because it is too high, compression the upper thoracic spine. Spine: The spine is again forced into an awkward ‘S’. This time the lumbar spine is being forced down then curving up and over the too-high pillow. This can again causes pain, aches, and exacerbate symptoms of existing spinal problems. Hips: With your lower hip now ‘down’ and your upper hip pulled up, we see that lower hip taking on more weight than it should. You really don’t want the hip joint and knee joints grinding together while you sleep, as it can weaken the capsule, joint, and connective tissues. Doctors recommend between 7-9 hours of sleep. Less than 6 hours a night and your brain is operating the same as it does with a .08 blood alcohol level. More than 9 hours and you are disrupting the delicate hormone cycle in your body. We talk about posture all the time, and how repetitive motions and postures can cause issues in the body. 7-9 hours is a long time to be out of alignment! It is hard to ‘even out’ in the morning and achieve a good posture.
Side sleeping does complicate things when picking a good pillow. Everyone has a different body shape so keep a few measurements in mind when picking the right pillow: neck girth, shoulder width, neck length, and distance from base of skull or ear to the top of the shoulder. This is why we support the Pillow-Wise pillow here at the office. We take these measurements of your body and take into account the position you sleep in, along with the firmness of your mattress and come up with the perfect pillow thickness for your specific situation. The best thing to do is get a custom-fitted pillow for your head, and also sleep with either a long body pillow or two smaller pillows for between your knees to take pressure of your hips, and under your arm to decompress the upper shoulder. The spine should be in alignment with your shoulders and hips even. This position will help your muscles relax the most, and you will get your best rest. |
The Norwalk Sports & Spine Blog is for answering your questions! Stay tuned to learn about our practice, health, food, treatments, and more!Subscribe for updates! Categories
All
Archives
May 2024
|










 RSS Feed
RSS Feed