 Understanding Degenerative Disc Disease: Causes, Symptoms, and Treatment Options In the realm of spinal health, few conditions are as commonly misunderstood yet impactful as degenerative disc disease (DDD). Despite its name, DDD is not actually a disease but a condition that affects the spinal discs as a result of natural wear and tear over time. Let's delve deeper into what degenerative disc disease entails, its causes, symptoms, and available treatment options. What is Degenerative Disc Disease? Degenerative disc disease refers to changes in the spinal discs, which act as cushions between the vertebrae in our spine. These discs are composed of a tough outer layer (annulus fibrosus) and a gel-like inner core (nucleus pulposus). As we age, these discs can degenerate or break down, leading to a variety of symptoms. Several factors contribute to the development of DDD: 1. Age: The primary risk factor is aging. As we grow older, the discs lose water content and elasticity, making them less effective as shock absorbers. 2. Genetics: Some people may have a genetic predisposition to developing DDD, where their discs naturally degenerate more rapidly. 3. Lifestyle Factors: Activities that place repetitive stress on the spine, such as heavy lifting, twisting motions, or excessive sitting, can accelerate disc degeneration. 4. Injuries: Trauma to the spine, such as from a fall or a sports injury, can also contribute to the development of DDD. Symptoms of Degenerative Disc Disease The symptoms of DDD can vary depending on the location and severity of the affected discs. Common symptoms include: - Pain: Typically in the lower back or neck, which may radiate to the buttocks or thighs. - Stiffness: Especially after prolonged sitting or standing. - Numbness or tingling: Along the nerve pathways affected by the degenerating discs. - Weakness: In the muscles served by the affected nerves. It's important to note that not everyone with degenerative disc changes experiences symptoms. In some cases, the degeneration is detected incidentally during imaging studies for other reasons. Conservative Treatments: - Chiropractic Treatment and Exercise: To strengthen the muscles supporting the spine and improve flexibility. - Activity Modification: Avoiding activities that worsen symptoms and adopting ergonomic practices. The choice of treatment depends on the severity of symptoms, the location of the affected discs, and the patient's overall health. Living with Degenerative Disc Disease While degenerative disc disease can be a chronic condition, many individuals manage their symptoms effectively through a combination of treatments and lifestyle adjustments. Maintaining a healthy weight, engaging in regular exercise that supports spinal health, and avoiding smoking (which can accelerate disc degeneration) are all beneficial strategies. Final Thoughts Degenerative disc disease is a prevalent condition that affects millions of people worldwide, often causing significant pain and discomfort. However, with proper diagnosis and a comprehensive treatment plan tailored to individual needs, many individuals can find relief and continue to lead active lives. If you suspect you may have degenerative disc disease or are experiencing persistent back or neck pain, consulting with a healthcare professional is essential for an accurate diagnosis and appropriate management plan. By understanding the complexities of degenerative disc disease, we can empower ourselves and others to take proactive steps towards spinal health and overall well-being.
0 Comments
 In today's digital age, many of us spend a significant portion of our day sitting at a computer, whether for work, leisure, or both. While technology has certainly improved our lives in many ways, it has also brought with it a host of health concerns. One common complaint that plagues computer users is neck pain. If you've ever wondered, "Why does my neck hurt when I sit at my computer too long?" you're not alone. In this blog post, we'll explore the reasons behind this discomfort and offer some tips on how to alleviate it. Poor Ergonomics: One of the leading causes of neck pain from prolonged computer use is poor ergonomics. Ergonomics refers to the science of designing and arranging objects so that people can interact with them efficiently and comfortably. When your computer setup is not ergonomically sound, it can put unnecessary strain on your neck and other body parts.Solution: Invest in an adjustable chair, a desk at the right height, and an ergonomic keyboard and mouse. Ensure that your monitor is at eye level, and your wrists and arms are in a neutral position while typing. Forward Head Posture: Another common issue is the development of forward head posture. This occurs when your head juts forward, causing your neck to carry more weight than it should. When you're engrossed in your computer screen, it's easy to let your head drift forward unconsciously. Solution: Be mindful of your posture. Regularly check that your head is aligned with your spine, not tilted forward. Some gentle neck and shoulder stretches can help counteract the effects of forward head posture. Prolonged Static Positions: Sitting in the same position for hours on end can lead to neck pain. Maintaining a static posture can put continuous pressure on the same muscles and joints, leading to discomfort and stiffness. Solution: Make an effort to take short breaks every 30-60 minutes. Stand up, stretch, and move around to prevent muscle fatigue. These breaks will not only benefit your neck but also your overall well-being. Screen Position: The position of your computer screen plays a crucial role in your neck's comfort. If your screen is too low or too high, it can force you to constantly tilt your head in an unnatural position, causing strain. Solution: Adjust your screen so that it is at or slightly below eye level. This will help keep your head and neck in a more neutral position. Stress and Tension: Stress can manifest physically in your body, often causing muscle tension and discomfort in the neck and shoulders. This tension can be exacerbated during long hours at the computer, especially if you're working on a demanding task. Neck pain from prolonged computer use is a common issue in our modern, technology-dependent world. However, with the right adjustments and practices, you can mitigate this discomfort and create a more ergonomic and comfortable workspace. Paying attention to your posture, taking regular breaks, and addressing the root causes of your pain can go a long way in ensuring that you can use your computer without the accompanying neck pain. Your health and comfort should always be a priority, so take the necessary steps to keep your neck happy and pain-free during those long hours at the computer. For many individuals, especially those dealing with chronic neck pain, chiropractic care can provide additional relief and support. Chiropractors are experts in assessing and treating musculoskeletal issues, including those related to the neck and spine. They can offer adjustments and manipulations that help restore proper alignment and alleviate tension in the neck and shoulders. Some benefits of chiropractic care for computer-related neck pain include:
 Plantar fasciitis, a common cause of heel pain, can be debilitating for those affected. It's characterized by inflammation of the thick band of tissue that runs across the bottom of your foot, connecting your heel bone to your toes. While various factors contribute to its development, recent studies have shed light on an unexpected association: the relationship between calf muscles and plantar fasciitis. Let's delve into this intriguing connection and explore what it means for both prevention and treatment strategies. Understanding Plantar Fasciitis: Before we explore the calf muscle connection, it's crucial to understand the mechanics of plantar fasciitis. The plantar fascia plays a vital role in supporting the arch of the foot and absorbing shock during walking, running, and other activities. When subjected to excessive stress or tension, tiny tears can develop in the fascia, leading to inflammation and pain, particularly around the heel. The Calf Muscle Link: Recent research has highlighted the role of calf muscles in the development and management of plantar fasciitis. The calf muscles, comprising the gastrocnemius and soleus, are integral to the function of the foot and ankle. Tightness or dysfunction in these muscles can alter biomechanics and increase strain on the plantar fascia, contributing to the development of plantar fasciitis. 1. Biomechanical Changes: Tight calf muscles can alter the mechanics of the foot and ankle, leading to overpronation or excessive inward rolling of the foot. This misalignment places greater stress on the plantar fascia, predisposing it to injury and inflammation. 2. Limited Range of Motion: Reduced flexibility in the calf muscles can restrict the ankle's range of motion, causing compensatory movements in the foot. These compensations can overload the plantar fascia, resulting in micro-trauma and subsequent pain. 3. Muscle Imbalance: Imbalances between the calf muscles and other muscles in the lower extremities can disrupt normal foot mechanics. Weakness or tightness in certain muscle groups may exacerbate tension on the plantar fascia, contributing to the development or persistence of plantar fasciitis. Prevention and Treatment Strategies: Understanding the relationship between calf muscles and plantar fasciitis can inform effective prevention and treatment strategies. Here are some approaches to consider: 1. Stretching Exercises: Regular stretching of the calf muscles can improve flexibility and reduce tension on the plantar fascia. Simple stretches such as calf raises, wall stretches, and towel stretches can be beneficial. 2. Strengthening Exercises: Strengthening exercises targeting the calf muscles and surrounding musculature can help correct imbalances and improve overall foot mechanics. Exercises like calf raises, toe curls, and ankle dorsiflexion exercises can be incorporated into a comprehensive rehabilitation program. 3. Footwear Modification: Wearing supportive footwear with adequate cushioning and arch support can help alleviate strain on the plantar fascia. Orthotic inserts or custom-made shoe inserts may also be beneficial in providing additional support and correcting biomechanical abnormalities. 4. Manual Therapy: Massage therapy, myofascial release, and trigger point therapy can help alleviate tightness and tension in the calf muscles, promoting optimal muscle function and reducing the risk of plantar fasciitis. 5. Gradual Progression: When increasing physical activity or introducing new exercises, it's essential to progress gradually to avoid overloading the calf muscles and plantar fascia. Sudden changes in intensity or volume can increase the risk of injury. Conclusion: The association between calf muscles and plantar fasciitis underscores the intricate interplay between muscle function and foot mechanics. By addressing calf muscle tightness, weakness, and imbalance, individuals can mitigate the risk of developing plantar fasciitis and improve outcomes for those already affected. Incorporating targeted stretching, strengthening, and therapeutic interventions into a comprehensive management plan can facilitate recovery and promote long-term foot health. As our understanding of this relationship continues to evolve, so too will our approaches to prevention and treatment, offering hope for those seeking relief from this common and often debilitating condition. Have you ever wondered what is actually “cracking” during a chiropractic manipulation? The audible “cracking” or “popping” sound that you hear during a manipulation is not that different from the sound you hear when you crack your knuckles. This sound actually has an official name, cavitation. And this cavitation is not your bones breaking, or ligaments snapping, but rather the quick release of gas that can occur within a joint. Many of our joints are what are classified as synovial joints- meaning there is a capsule that exists within the joint along with synovial fluid. Synovial fluid is the natural lubrication that occurs within a joint allowing it to move pain-free. Restrictions in joint mobility, often due to misalignments or adhesions, can contribute to the build-up of gas. When a joint is not moving through its full range of motion, the synovial fluid becomes stagnant, allowing gas to accumulate over time. Thus, the more restricted an area of your spine is, the more pressure that develops there. This pressure can be felt as loss of ROM, pain, tension, etc. During a chiropractic adjustment, or manipulation, your joints get stretched near their end range. This can allow for a myriad of things to ensue like relaxation of the surrounding musculature, but more excitingly, the cavitation. When a joint capsule is stretched it creates a negative pressure within the capsule leading to the formation and collapse of gas bubbles. These gas bubbles are mainly nitrogen and materialize as the gas is pulled out of solution by the negative pressure that happens as a result of the capsule stretching. So what does this mean- is my adjustment not working if there’s no sound? Cavitations can vary between people, and can even vary depending on the body part in the same individual. Oftentimes cavitations occur without the added force of a chiropractic adjustment, like when you’re moving after sitting down for a long time. The effectiveness of a chiropractic manipulation is not determined by how loud a cavitation is, contrary to popular belief. There are no known downsides or risks associated with the frequency of a cavitation within a particular joint, or even how loud a cavitation is at this time. The “cracking” or “popping” sound is just a bonus!  Phase II Exercise: Single Leg RDL with foam roller assist Phase II Exercise: Single Leg RDL with foam roller assist What are the “hamstrings”? The hamstrings are a bundle of three separate muscles: semimembranosus, semitendinosus, and biceps femoris. All three of them are located on the back of the thigh. The main action of these muscles is to bend, or flex, the knee as well as internally rotate and adduct the leg. Injuries to this muscle group are extremely common unfortunately, and can happen to individuals of all activity levels; however 29% of sports injuries can be classified as hamstring strain injuries. Usually people will feel the onset of pain while running or sprinting and can hear or feel an audible pop. Bruising is also not uncommon depending on the severity of the strain. These injuries are very susceptible to a risk of reinjury, so it’s essential to determine the true cause of the injury. Whether it be due to a muscle imbalance with the quadriceps, or a lack of flexibility and strength. Little evidence exists to show that over the counter anti-inflammatory medications are beneficial as well. Low level laser therapy, and working on the appropriate rehabilitation plan can provide long-term effects. With rehabilitation the goal is to address the biomechanical dysfunction that led to the initial injury. Eccentric strengthening has been shown to be the most effective at reducing re-injury. Eccentric contractions occur when the muscle is being activated while also lengthened at the same time. In addition to eccentric strengthening of the hamstrings, working on core and lumbo-pelvic stability and balance should be a focal point. The initial phase of rehabilitation begins immediately after the injury and can last for four weeks. In this phase regular activity should be modified to reduce extraneous stress on the tissue, however movement and mild exercise can prevent full atrophy and decreased neural drive. In this phase exercises will be geared towards range of motion and include mainly open-kinetic chain movements. The second phase of rehabilitation aims to restore maximal strength contractions with pain-free repetitions. This second phase can last for several weeks. The third, and final, phase includes dynamic and advanced exercises to re-establish athletic movements in full capacity. The overall prognosis of hamstring strain injuries is very good as long as the appropriate rehabilitation is performed. Phase I Exercises
Phase II Exercises
Phase III Exercises
-Danirose Billings 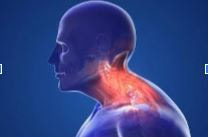 A Dowager's hump, also known as kyphosis or hyperkyphosis, refers to an excessive outward curvature of the upper spine, resulting in a rounded hump-like appearance in the upper back and neck. While reversing a Dowager's hump entirely is not always possible, there are measures individuals can take to improve posture, strengthen muscles, and potentially reduce the prominence of the hump. The best medicine of course would be the avoidance of developing such a hump in the first place. A hyperkyphosis can lead to other significant problems such as headaches, neck pain, numbness/tingling, spinal stenosis, disc herniations/bulges, spinal degeneration and arthritis. Prevention and Management Strategies 1. Posture Correction:
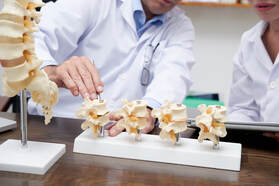 Image by pressfoto on Freepik Image by pressfoto on Freepik In our quest for optimal health and wellness, we often focus on nutrition, exercise, and mindfulness practices. However, there's one crucial aspect of wellness that is sometimes overlooked: chiropractic maintenance care. Chiropractic care isn't just for alleviating pain; it's a cornerstone of preventive healthcare that can unlock a host of benefits for both body and mind. Chiropractic care is founded on the principle that proper alignment of the spine is essential for the body to function optimally. Through adjustments and other manual techniques, chiropractors aim to restore alignment, relieve pressure on nerves, and facilitate the body's natural ability to heal itself. While many people seek chiropractic care to address specific issues like back pain, neck pain, or headaches, maintenance care takes a proactive approach. Rather than waiting for symptoms to arise, individuals engage in regular chiropractic visits to maintain spinal health and prevent future problems. Just as we service our cars regularly to prevent breakdowns, our bodies also benefit from routine maintenance. Here's why regular chiropractic care is so vital:
If you're new to chiropractic care or considering incorporating maintenance visits into your wellness routine, here are a few tips to get started:
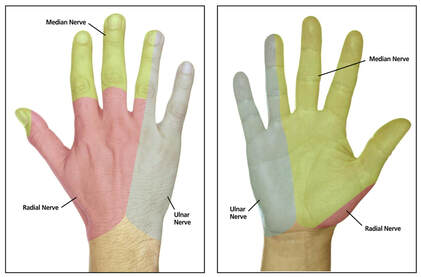
TEXT or call 203-842-88502 to schedule your chiropractic "tune-up" today! -- By Erica Sastre, LMT  YES Understanding Carpal Tunnel: Carpal tunnel syndrome is characterized by numbness, tingling, or pain in the hands (particularly the thumb, index finger, middle finger and the thumb side of the ring finger, as this is the part of the hand innervated by the median nerve). The irritation or pain can also refer up the arm, affecting more than just the hand and wrist. The onset might be during sleep, after prolonged activity, or seemingly random. Persistence or recurrence of these symptoms should definitely be addressed! Un-addressed carpal tunnel will lead to a steady increase in these symptoms, and eventually weakness and atrophy of the hands. True Carpal Tunnel is an irritation of the median nerve at the transverse carpal ligament. Carpal tunnel affects about 1 in 10 people, making it the most common nerve compression syndrome! Carpal tunnel syndrome often affects, machinists, hairdressers, musicians, massage therapists, even chiropractors! Anyone making prolonged repetitive use of their hands, fingers and wrists. Now that everyone is texting and typing as much as typists used to when this syndrome was identified... It can really affect anyone. 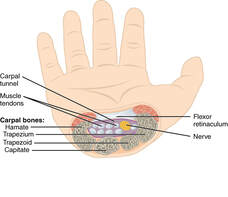 Understanding Nerve Compression Syndromes: When you have symptoms of numbness or tingling, this usually indicates a nerve problem. Nerves run from the spine throughout the body to give us sensation and feeling, giving our brains vital information about the world around us. When a nerve is compressed or pinched, it interferes with these signals. This is what happens when your arm or foot falls asleep after sitting on it for a long time. Except with carpal tunnel you can’t quite shake it out the way you can a sleeping foot. The more frequent and persistent numbness and tingling become the more severe the problem is. Carpal Tunnel Syndrome specifically compresses the median nerve at the wrist. There are other syndromes that have the same symptoms as carpal tunnel, for example, the median nerve can be compressed at the elbow such as in pronator teres syndrome, or at the shoulder such as in thoracic outlet syndrome, or in the neck due to a subluxation or misalignment in the cervical spine. That is why it is important to get a proper diagnosis for your symptoms. There have been many cases of patients receiving surgery for carpal tunnel but, the surgery did noting for their symptoms as they actually had one of these other conditions. What's happening in the 'tunnel'? The transverse carpal ligament is a round band of fascia that hold the flexor muscles in place. Imagine a rubbery calamari ring in your wrist, and that your muscles and nerves are strands of spaghetti strands are running through it! (Are you hungry yet?) The wrist is a high traffic area! You’ve got carpal bones, you’ve got the tendons of the flexor muscles, you’ve got the median nerve… When this area gets over-crowded the other tissues in the space will compress the median nerve and cause these symptoms. There are several things that can cause a jam-up in this area include edema, subluxation of a carpal bone, fascial adhesion, inflammation of the flexor muscle tendons, and inflammation of the transverse carpal ligament itself. How can this condition be treated? Manual therapy can be really effective in treating carpal tunnel. Calming the overworked tissues, reducing inflammation, breaking fascia and adhesions, and reducing pain. Massage, acupuncture, chiropractic adjustment of the wrist, stretches and exercises, using a wrist brace to splint the wrist, resting the wrist, cortisol shots, and even surgery are all options. Should I get evaluated for carpal tunnel? You can give yourself the following simple tests: If any of the above exercises causes numbness, tingling, or pain in the hands, make an appointment to get checked for carpal tunnel.
Fun Facts:
That's a wrap for our blog this week! We hoped you learned a little more about this common condition. Stay tuned for our next blog, and send your questions to [email protected] --- By Erica Sastre, LMT  Yes! Chiropractic has been proven to help manage both acute and chronic pain. Pain management, in general, is a big issue in healthcare. Let’s look at some facts: Low back pain is the single leading cause of disability. According to the US bone and Joint initiative study, back pain was cause for over 264 million days off of work. That is all without considering any other type of chronic pain condition. Pain affects more Americans than diabetes, heart disease and cancer combined. When looking for solutions to chronic pain, the first thing we tend to reach for is over-the-counter aids such as Aspirin, Advil, or Ibuprofen. Then if these conditions worsen and we go to the doctor we are typically directed to stronger prescription medications, which, can be concerning to many patient situations. Many people are looking for ways to treat their chronic pain without resorting to drugs of the traditional medication protocol. With alternative care we can lessen our dependency on over the counter drugs and even opioids.  Back pain is also one of the most common conditions that opioids are prescribed for with over half of opioid users reporting back pain among their symptoms. Why is this connection between back pain and opioids so concerning? While prescription opioids are certainly helpful to many patients in complex severe conditions, however, we need to also be looking at the big picture of the opioid crisis: In 2016, illicit and prescription opioids were responsible for more than 42,000 fatal overdoses across the country. According to the Centers of Disease Control and Prevention, those numbers have quintupled since 1999, which means the problem is just getting worse. The good news is that, alternative medicines are already making great improvements to these dire statistics.  Let's take a look at some strategies the VA has been using in order reduce opioid addiction among veterans. After launching one initiative, they were able to reduce overall opioid prescriptions by 41% over the past five years. The project was focused on non-drug treatment for chronic pain, such as acupuncture, spinal manipulation therapy, chiropractic care, and yoga. It is also good news to know that patients who received services from a chiropractor were less likely to fill a prescription for opioid medication, and, there was a 51 percent lower likelihood of an adverse drug incident compared to non recipients of chiropractic care.  A visit to the chiropractor may also be more cost effective for sufferers of chronic pain. In one study, "those who initiated treatment for low back pain with chiropractic rather than a regular MD had 40% in reduced healthcare cost!" In general “Healthcare plans that incorporate chiropractic typically realize a 2:1 return for every dollar spent.” There are numerous research studies, reports, and surveys proving how effective chiropractic can be for pain: "In a Randomized controlled trial, 183 patients with neck pain were randomly allocated to manual therapy (spinal mobilization), physiotherapy (mainly exercise) or general practitioner care (counseling, education and drugs) in a 52-week study. The clinical outcomes measures showed that manual therapy resulted in faster recovery than physiotherapy and general practitioner care. Moreover, total costs of the manual therapy-treated patients were about one-third of the costs of physiotherapy or general practitioner care." Korthals-de Bos et al (2003), British Medical Journal “Patients with chronic low-back pain treated by chiropractors showed greater improvement and satisfaction at one month than patients treated by family physicians. Satisfaction scores were higher for chiropractic patients. A higher proportion of chiropractic patients (56 percent vs. 13 percent) reported that their low-back pain was better or much better, whereas nearly one-third of medical patients reported their low-back pain was worse or much worse.” Nyiendo et al (2000), Journal of Manipulative and Physiological Therapeutic The evidence and anecdotes are solid. If you are suffering form chronic or acute pain, chiropractic care may well worth a try! Send us your questions! Yours might be answered next week. [email protected] Sources and Further Reading:
NIH Fact Sheet -- Pain Management The Center for Disease Control and Prevention -- Drug Overdose Deaths VHA Pain Management -- Opioid Saftey Initiative Boss Magazine -- Corrective Care for the Opioid Epidemic American Chiropractic Association -- What Research Shows About Chiropractic -- By Erica Sastre, LMT 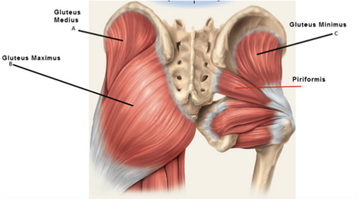 Did your massage therapist hit a particularly tender spot in your glutes? Did you have pain or tingling running down your leg? Why is your chiropractor trying to make you do so many squats? This week we are putting the spotlight on the piriformis muscle! The piriformis muscle is a muscle under the gluteus maximus, it attaches at the anterior surface of the sacrum, and the superior aspect of the greater trochanter (SI joint to the top of the femur). It Latterally rotates the hip (twists your thigh outward) , and abducts the hip when the hip his flexed (pulls your thigh away from the body center-line). 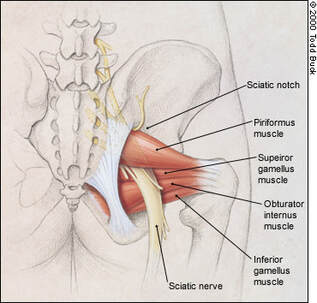 What could possibly go wrong? Piriformis can be a literal pain-in-the-butt! A tight or knotted up piriformis muscle can cause pain on its own, or limit strength and flexibility. However, this small muscle can cause much bigger problems. The Piriformis is often to blame for sciatic pain symptoms. The sciatic nerve runs right past the piriformis muscle, and sometimes even through the piriformis muscle. Due to its placement in the body, tightness in the piriformis and adjacent muscles can pinch the sciatic nerve. This can send pain, numbness, or tingling down all or parts of the leg! If you have ruled out a spinal issues as your source of sciatic, it's time to address the piriformis muscle. How does the piriformis affect my posture? Check out your toes! If your feet tend to turn in when you are standing, walking, running, or squatting you may have a weak piriformis muscle. Likewise, if you see that your feet tend to turn outward when standing, walking, running, or squatting, it may be a sign that your piriformis is overdoing it. Either one of these postures can cause problems in the legs, hips and knees, especially with load-bearing exercise. Squatting and lifting weights with misalignment can spell disaster for the knees! Keep in mind that if it is a hip/piriformis weakness, the positional problem will originate from where the hip and thigh meet. If the positional problem originates in the knee or ankle, we will have other muscles to look at! That's why it's a good idea to see a professional, like your chiropractor, to help evaluate postural problems. How do I stretch it? Pigeon pose is everyone’s favorite piriformis stretch! There are a number of modified pigeon poses you can try if you are less flexible. If floor stretches are uncomfortable, try doing a pigeon pose on a chair, couch, or low table. The 'figure 4' can be done sitting or supine (on your back), or even standing if you have good balance! How do I strengthen it? Piriformis is a lateral rotator. Meaning, it twists the thigh 'outward' from your hip. Working the gluteal region will generally build the piriformis, as well as create support for the piriformis with the other gluteal muscles. Squats are an easy way to develop the glutes. Add a band for extra resistance! Try a one-legged dead lift and keep in mind that the grounded leg is the piriformis that you are strengthening. Work one leg at a time, grab on to the back of a chair, bar, or ledge. Lift the other leg out to the side, you can do this exercise with your feet paralell (both toes facing forward) or 'turned out' (feet make a V shape with your toes pointing outward, like in ballet). Try this one with a band as well! 'Fire Hydrant' starts on all fours. Keep your knee at 90 degrees then swing your leg out to the side, keeping your frame strong to isolate and work the glutes. Fun facts about the piriformis
The piriformis is only one of six muscles in the lateral rotator group. The others are; gemellus superior, obturator internus, gemellus inferior, quadratus femoris and the obturator externus. In 17% of the population the piriformis muscle is pierced by all or part of the sciatic nerve. The word piriformis comes from latin, meaning ‘pear shaped’. Hopefully you learned something fun about the piriformis today! Stay tuned for our next Q&A, and send your questions to [email protected]! What muscle should we feature next? |
The Norwalk Sports & Spine Blog is for answering your questions! Stay tuned to learn about our practice, health, food, treatments, and more!Subscribe for updates! Categories
All
Archives
May 2024
|









 RSS Feed
RSS Feed